Marijuana
List of Controlled Substances
Lists of Scheduling Actions, Controlled Substances, Regulated Chemicals (PDF) (May 2019)
This document is a general reference and not a comprehensive list. This list describes the basic or parent chemical and does not describe the salts, isomers and salts of isomers, esters, ethers and derivatives which may also be controlled substances.
| Scheduling Actions | Controlled Substances | List I and II Regulated Chemicals |
|---|---|---|
| Alphabetical Order | Alphabetical Order | Alphabetical Order |
| Chronological Order | DEA Drug Code Number | DEA Number |
| CSA Schedule | List Number | |
| Illicit Uses and Threshold Quantities |
Exempted Lists
Exempt Anabolic Steroid Products
Exempt Anabolic Steroid Products Procedures
Exempt Anabolic Steroid Products List (PDF) (February 6, 2015)
Exempt Chemical Preparations
Exempt Chemical Preparations List (PDF) (November 7, 2017) For Application Dates Through December 31, 2016
Exempted Prescription Products
Exempted Prescription Products Application
Exempted Prescription Products List (PDF) (February 28, 2019)
Lists of Controlled Substances Disclaimer
Section 812 of the Controlled Substances Act (21 U.S.C. §801 et seq.) (CSA) lists substances which were controlled in 1970 when the CSA was enacted. Since then many substances have been added, removed, or transferred from one schedule to another. The current list of controlled substances can be found in section 1308 of the most recent issue of Title 21 Code of Federal Regulations (CFR) Part 1300 to end (21 CFR §1308) and the final rules which were published in the Federal Register subsequent to the issuance of the CFR.
These lists describe the basic or parent chemical and do not describe the salts, isomers, salts of isomers, esters, ethers, and derivatives which may be controlled substances. These are not comprehensive lists so please note that a substance need not be listed as a controlled substance to be treated as a scheduled substance for criminal prosecution. The 'Other Names' column, provides some examples of alternate names for certain compounds, and in some instances provides examples of 'positional isomers'. If outside parties want to ensure that a compound is not considered a scheduled substance or listed chemical, they should write the DEA, Drug and Chemical Evaluation Section (DRE), Diversion Control Division, 8701 Morrissette Drive, Springfield, Virginia 22152, for an official determination.
A substance (not included on these lists) may also be regulated as a controlled substance analogue. A controlled substance analogue is a substance which is intended for human consumption, is structurally substantially similar to a schedule I or schedule II substance, is pharmacologically substantially similar to a schedule I or schedule II substance, or is represented as being similar to a schedule I or schedule II substance and is not an approved medication in the United States. See 21 U.S.C. §802(32)(A) for the definition of a controlled substance analogue and 21 U.S.C. §813 for the schedule.
Defined Abbreviations
| Defined Abbreviation | Controlled Substance Analogue |
|---|---|
| 2C-B | 4-Bromo-2,5-dimethoxyphenethylamine |
| 2C-T-7 | 2,5-Dimethoxy-4(n)-propylthiophenethylamine |
| BZP | N-Benzylpiperazine |
| DMT | Dimethyltryptamine |
| DOM | 4-Methyl-2,5-dimethoxyamphetamine |
| GBL | Gamma butyrolactone |
| GHB | Gamma hydroxybutyric acid, gamma hydroxybutyrate, 4-hydroxybutanoic acid, sodium oxybate |
| LAAM | Levo-alphacetylmethadol |
| LSD | Lysergic acid diethylamide, lysergide |
| MDA | 3,4-Methylenedioxyamphetamine |
| MDE | 3,4-Methylenedioxy-N-ethylamphetamine |
| MDMA | 3,4-Methylenedioxymethamphetamine |
| MPPP | 1-Methyl-4-phenyl-4-propionoxypiperidine |
| P2P | Phenyl-2-propanone, phenylacetone |
| PCC | 1-Piperidinocyclohexanecarbonitrile |
| PCE | N-Ethyl-1-phenylcyclohexylamine |
| PCH | 1-Phenylcyclohexylamine |
| PCP | 1-(1-Phenylcyclohexyl)piperidine, phencyclidine |
| PEPAP | 1-(2-Phenylethyl)-4-phenyl-4-acetoxypiperidine |
| PHP | 1-(1-Phenylcyclohexyl)pyrrolidine |
| SPA | (-)-1-Dimethylamino-1,2-diphenylethane |
| TCP | 1-[1-(2-Thienyl)cyclohexyl]piperidine |
| TCPy | 1-[1-(2-Thienyl)cyclohexyl]pyrrolidine |
| THC | Tetrahydrocannabinols |
| THG | Tetrahydrogestrinone |
Definition of Controlled Substance Schedules
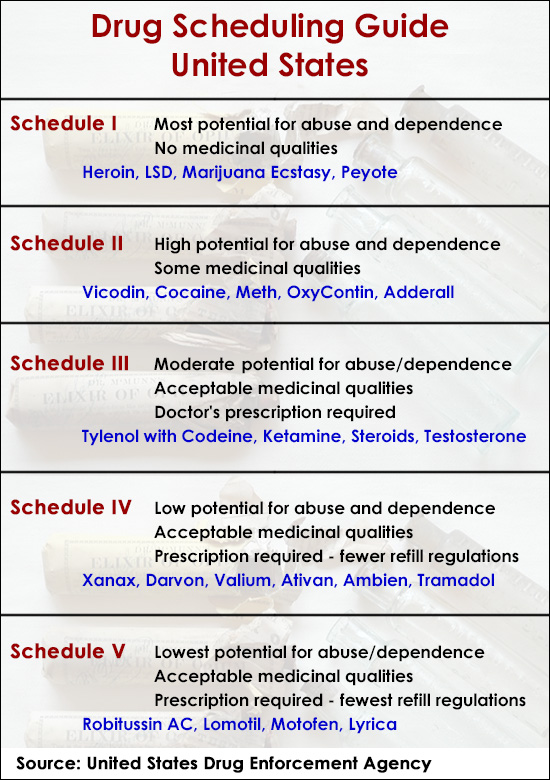
Drugs and other substances that are considered controlled substances under the Controlled Substances Act (CSA) are divided into five schedules. An updated and complete list of the schedules is published annually in Title 21 Code of Federal Regulations (C.F.R.) §§ 1308.11 through 1308.15. Substances are placed in their respective schedules based on whether they have a currently accepted medical use in treatment in the United States, their relative abuse potential, and likelihood of causing dependence when abused. Some examples of the drugs in each schedule are listed below.
Schedule I Controlled Substances
Substances in this schedule have no currently accepted medical use in the United States, a lack of accepted safety for use under medical supervision, and a high potential for abuse.
Some examples of substances listed in Schedule I are: heroin, lysergic acid diethylamide (LSD), marijuana (cannabis), peyote, methaqualone, and 3,4-methylenedioxymethamphetamine ('Ecstasy').
Schedule II/IIN Controlled Substances (2/2N)
Substances in this schedule have a high potential for abuse which may lead to severe psychological or physical dependence.
Examples of Schedule II narcotics include: hydromorphone (Dilaudid®), methadone (Dolophine®), meperidine (Demerol®), oxycodone (OxyContin®, Percocet®), and fentanyl (Sublimaze®, Duragesic®). Other Schedule II narcotics include: morphine, opium, codeine, and hydrocodone.
Examples of Schedule IIN stimulants include: amphetamine (Dexedrine®, Adderall®), methamphetamine (Desoxyn®), and methylphenidate (Ritalin®).
Other Schedule II substances include: amobarbital, glutethimide, and pentobarbital.
Schedule III/IIIN Controlled Substances (3/3N)
Substances in this schedule have a potential for abuse less than substances in Schedules I or II and abuse may lead to moderate or low physical dependence or high psychological dependence.
Examples of Schedule III narcotics include: products containing not more than 90 milligrams of codeine per dosage unit (Tylenol with Codeine®), and buprenorphine (Suboxone®).
Examples of Schedule IIIN non-narcotics include: benzphetamine (Didrex®), phendimetrazine, ketamine, and anabolic steroids such as Depo®-Testosterone.
Schedule IV Controlled Substances
Class 2 Prescription Drugs
Substances in this schedule have a low potential for abuse relative to substances in Schedule III.
Examples of Schedule IV substances include: alprazolam (Xanax®), carisoprodol (Soma®), clonazepam (Klonopin®), clorazepate (Tranxene®), diazepam (Valium®), lorazepam (Ativan®), midazolam (Versed®), temazepam (Restoril®), and triazolam (Halcion®).
Schedule V Controlled Substances
Substances in this schedule have a low potential for abuse relative to substances listed in Schedule IV and consist primarily of preparations containing limited quantities of certain narcotics.
Examples of Schedule V substances include: cough preparations containing not more than 200 milligrams of codeine per 100 milliliters or per 100 grams (Robitussin AC®, Phenergan with Codeine®), and ezogabine.
RESOURCES > Chemical Control Program > List I and List II Chemicals
Congress passed the Chemical Diversion and Trafficking Act (CDTA) in 1988 and subsequent amendments placed under control 41 chemicals. These laws provide a system of regulatory controls and criminal sanctions to address both domestic and international diversion of important chemicals without interrupting access to chemicals destined for legitimate commerce. The CDTA created two categories for the controlled chemicals, as follows:
List I Chemicals
List II Chemicals
Drugs affecting the cardiac action potential. The sharp rise in voltage ('0') corresponds to the influx of sodium ions, whereas the two decays ('1' and '3', respectively) correspond to the sodium-channel inactivation and the repolarizing efflux of potassium ions. The characteristic plateau ('2') results from the opening of voltage-sensitive calcium channels.
Antiarrhythmic agents, also known as cardiac dysrhythmia medications, are a group of pharmaceuticals that are used to suppress abnormal rhythms of the heart (cardiac arrhythmias), such as atrial fibrillation, atrial flutter, ventricular tachycardia, and ventricular fibrillation.
Many attempts have been made to classify antiarrhythmic agents. The problem arises from the fact that many of the antiarrhythmic agents have multiple modes of action, making any classification imprecise.
- 1Vaughan Williams classification
Vaughan Williams classification[edit]
The Vaughan Williams classification was introduced in 1970 by Miles Vaughan Williams.[1]
Miles was the tutor for Pharmacology at Hertford College, Oxford; one of his students, Bramah N. Singh,[2] contributed to the development of the classification system, and had a subsequent eminent career in the United States; the system is therefore sometimes known as the Singh-Vaughan Williams classification.
The five main classes in the Vaughan Williams classification of antiarrhythmic agents are:
- Class I agents interfere with the sodium (Na+) channel.
- Class II agents are anti-sympathetic nervous system agents. Most agents in this class are beta blockers.
- Class III agents affect potassium (K+) efflux.
- Class IV agents affect calcium channels and the AV node.
- Class V agents work by other or unknown mechanisms.
With regard to management of atrial fibrillation, classes I and III are used in rhythm control as medical cardioversion agents, while classes II and IV are used as rate-control agents.
| Class | Known as | Examples | Mechanism | Medical uses [3] |
|---|---|---|---|---|
| Ia | Fast-channel blockers | (Na+) channel block (intermediate association/dissociation) and K+ channel blocking effect; affects QRS complex class 1a prolong the action potential and has intermediate effect on the 0 phase of depolarization |
| |
| Ib | Na+ channel block (fast association/dissociation); can prolong QRS complex in overdose class 1b shorten the action potential of myocardial cell and has weak effect on intiation of phase 0 of depolarization |
| ||
| Ic | Na+ channel block (slow association/dissociation) has no effect on action potential and has the strongest effect on initiation phase 0 the depolarization |
| ||
| II | Beta-blockers | Beta blocking Propranolol also shows some class I action |
| |
| III | K+ channel blocker Sotalol is also a beta blocker[4]Amiodarone has Class III mostly, but also I, II, & IV activity[5] |
| ||
| IV | Calcium Channel Blockers | Ca2+ channel blocker |
| |
| V | Work by other or unknown mechanisms (direct nodal inhibition) | Used in supraventricular arrhythmias, especially in heart failure with atrial fibrillation, contraindicated in ventricular arrhythmias. Or in the case of magnesium sulfate, used in torsades de pointes. |
Class I agents[edit]
The class I antiarrhythmic agents interfere with the sodium channel.Class I agents are grouped by what effect they have on the Na+ channel, and what effect they have on cardiac action potentials.
Class I agents are called membrane-stabilizing agents, 'stabilizing' referring to the decrease of excitogenicity of the plasma membrane which is brought about by these agents. (Also noteworthy is that a few class II agents like propranolol also have a membrane stabilizing effect.)
Class I agents are divided into three groups (Ia, Ib, and Ic) based upon their effect on the length of the action potential.[8][9]
- Ia lengthens the action potential (right shift)
- Ib shortens the action potential (left shift)
- Ic does not significantly affect the action potential (no shift)
- Class Ia
- Class Ib
- Class Ic
Class II agents[edit]
Class II agents are conventional beta blockers. They act by blocking the effects of catecholamines at the β1-adrenergic receptors, thereby decreasing sympathetic activity on the heart, which reduces intracellular cAMP levels and hence reduces Ca2+ influx. These agents are particularly useful in the treatment of supraventricular tachycardias. They decrease conduction through the AV node.
Class II agents include atenolol, esmolol, propranolol, and metoprolol.
Class III agents[edit]
Class III
Class III agents predominantly block the potassium channels, thereby prolonging repolarization.[10] Since these agents do not affect the sodium channel, conduction velocity is not decreased. The prolongation of the action potential duration and refractory period, combined with the maintenance of normal conduction velocity, prevent re-entrant arrhythmias. (The re-entrant rhythm is less likely to interact with tissue that has become refractory). The class III agents exhibit reverse-use dependence (their potency increases with slower heart rates, and therefore improves maintenance of sinus rhythm). Inhibiting potassium channels, slowing repolarization, results in slowed atrial-ventricular myocyte repolarization. Class III agents have the potential to prolong the QT interval of the EKG, and may be proarrhythmic (more associated with development of polymorphic VT).
Class III agents include: bretylium, amiodarone, ibutilide, sotalol, dofetilide, vernakalant and dronedarone.
Class IV agents[edit]
Class IV agents are slow non-dihydropyridinecalcium channel blockers. They decrease conduction through the AV node, and shorten phase two (the plateau) of the cardiac action potential. They thus reduce the contractility of the heart, so may be inappropriate in heart failure. However, in contrast to beta blockers, they allow the body to retain adrenergic control of heart rate and contractility.
Class IV agents include verapamil and diltiazem.
Class V / other agents[edit]
Since the development of the original Vaughan Williams classification system, additional agents have been used that do not fit cleanly into categories I through IV.
Agents include:
- Digoxin, which decreases conduction of electrical impulses through the AV node and increases vagal activity via its central action on the central nervous system, via indirect action, leads to an increase in acetylcholine production, stimulating M2 receptors on AV node leading to an overall decrease in speed of conduction.
- Adenosine is used intravenously for terminating supraventricular tachycardias.[11]
- Magnesium sulfate, an antiarrhythmic drug, but only against very specific arrhythmias [12] which has been used for torsades de pointes.[13][14]
- Trimagnesium dicitrate (anhydrous) as powder or powder caps in pure condition, better bioavailability than ordinary MgO[15]
History[edit]
The initial classification system had 4 classes, although their definitions different from the modern classification. Those proposed in 1970 were:[1]

- Drugs with a direct membrane action: the prototype was quinidine, and lignocaine was a key example. Differing from other authors, Vaughan-Williams describe the main action as a slowing of the rising phase of the action potential.
- Sympatholytic drugs (drugs blocking the effects of the sympathetic nervous system): examples included bretylium and adrenergic beta-receptors blocking drugs. This is similar to the modern classification, which focuses on the latter category.
- Compounds that prolong the action potential: matching the modern classification, with the key drug example being amiodarone, and a surgical example being thyroidectomy. This was not a defining characteristic in an earlier review by Charlier et al. (1968),[16] but was supported by experimental data presented by Vaughan Williams (1970).[1]:461 The figure illustrating these findings was also published in the same year by Singh and Vaughan Williams.[17]
- Drugs acting like dephenylhydantoin (DPH): mechanism of action unknown, but others had attributed its cardiac action to an indirect action on the brain;[18] this drug is better known as antiepileptic drug phenytoin.
Sicilian gambit classification[edit]
Another approach, known as the 'Sicilian gambit', placed a greater approach on the underlying mechanism.[19][20][21]
It presents the drugs on two axes, instead of one, and is presented in tabular form. On the Y axis, each drug is listed, in roughly the Singh-Vaughan Williams order. On the X axis, the channels, receptors, pumps, and clinical effects are listed for each drug, with the results listed in a grid. It is, therefore, not a true classification in that it does not aggregate drugs into categories.[22]
A modernized Oxford classification by Lei, Huang, Wu and Terrar[edit]
A recent publication has now emerged with a fully modernised drug classification.[23] This preserves the simplicity of the original Vaughan Williams framework while capturing subsequent discoveries of sarcolemmal, sarcoplasmic reticular and cytosolic biomolecules. The result is an expanded but pragmatic classification that encompasses approved and potential anti-arrhythmic drugs. This will aid our understanding and clinical management of cardiac arrhythmias and facilitate future therapeutic developments. It starts by considering the range of pharmacological targets, and tracks these to their particular cellular electrophysiological effects. It retains but expands the original Vaughan Williams classes I to IV, respectively covering actions on Na+ current components, autonomic signalling, K+ channel subspecies, and molecular targets related to Ca2+ homeostasis. It now introduces new classes incorporating additional targets, including:
- Class 0: ion channels involved in automaticity
- Class V: mechanically sensitive ion channels
- Class VI: connexins controlling electrotonic cell coupling
- Class VII: molecules underlying longer term signalling processes affecting structural remodeling.
It also allows for multiple drug targets/actions and adverse pro-arrhythmic effects. The new scheme will additionally aid development of novel drugs under development and is illustrated below.
- Common anti-arrhythmic drugs under the modernized classification according to Lei et al 2018.
See also[edit]
- Cardiac Arrhythmia Suppression Trial (CAST)
References[edit]
- ^ abcVaughan Williams, EM (1970) Classification of antiarrhythmic drugs. In Symposium on Cardiac Arrhythmias (Eds. Sandoe E, Flensted- Jensen E, Olsen KH). Astra, Elsinore. Denmark (1970)
- ^Kloner RA (2009). 'A Salute to Our Founding Editor-in-Chief Bramah N. Singh, MD, DPhil, DSc, FRCP'. Journal of Cardiovascular Pharmacology and Therapeutics. 14 (3): 154–56. doi:10.1177/1074248409343182. PMID19721129.
- ^Unless else specified in boxes, then ref is: Rang, H. P. (2003). Pharmacology. Edinburgh: Churchill Livingstone. ISBN978-0-443-07145-4.[page needed]
- ^Kulmatycki KM, Abouchehade K, Sattari S, Jamali F (May 2001). 'Drug-disease interactions: reduced beta-adrenergic and potassium channel antagonist activities of sotalol in the presence of acute and chronic inflammatory conditions in the rat'. Br. J. Pharmacol. 133 (2): 286–94. doi:10.1038/sj.bjp.0704067. PMC1572777. PMID11350865.
- ^Waller, Derek G.; Sampson, Tony (2013). Medical Pharmacology and Therapeutics E-Book. Elsevier Health Sciences. p. 144. ISBN9780702055034.
- ^'treatment of paroxysmal atrial fibrillation - General Practice Notebook'. www.gpnotebook.co.uk.
- ^'protocol for management of haemodynamically stable ventricular tachycardia – General Practice Notebook'. www.gpnotebook.co.uk. Retrieved 2016-02-09.
- ^Milne JR, Hellestrand KJ, Bexton RS, Burnett PJ, Debbas NM, Camm AJ (February 1984). 'Class 1 antiarrhythmic drugs – characteristic electrocardiographic differences when assessed by atrial and ventricular pacing'. Eur. Heart J. 5 (2): 99–107. doi:10.1093/oxfordjournals.eurheartj.a061633. PMID6723689.
- ^Trevor, Anthony J.; Katzung, Bertram G. (2003). Pharmacology. New York: Lange Medical Books/McGraw-Hill, Medical Publishing Division. p. 43. ISBN978-0-07-139930-2.
- ^Lenz, TL; Hilleman, DE (2000). 'Dofetilide, a New Class III Antiarrhythmic Agent'. Pharmacotherapy. 20 (7): 776–86. doi:10.1592/phco.20.9.776.35208. PMID10907968.
- ^Conti JB, Belardinelli L, Utterback DB, Curtis AB (March 1995). 'Endogenous adenosine is an antiarrhythmic agent'. Circulation. 91 (6): 1761–67. doi:10.1161/01.cir.91.6.1761. PMID7882485.
- ^Brugada P (July 2000). 'Magnesium: an antiarrhythmic drug, but only against very specific arrhythmias'. Eur. Heart J. 21 (14): 1116. doi:10.1053/euhj.2000.2142. PMID10924290.
- ^Hoshino K, Ogawa K, Hishitani T, Isobe T, Eto Y (October 2004). 'Optimal administration dosage of magnesium sulfate for torsades de pointes in children with long QT syndrome'. J Am Coll Nutr. 23 (5): 497S–500S. doi:10.1080/07315724.2004.10719388. PMID15466950.
- ^Hoshino K, Ogawa K, Hishitani T, Isobe T, Etoh Y (April 2006). 'Successful uses of magnesium sulfate for torsades de pointes in children with long QT syndrome'. Pediatr Int. 48 (2): 112–17. doi:10.1111/j.1442-200X.2006.02177.x. PMID16635167.
- ^Lindberg JS, Zobitz MM, Poindexter JR, Pak CY (1990). 'Magnesium bioavailability from magnesium citrate and magnesium oxide'. Journal of the American College of Nutrition. 9 (1): 48–55. doi:10.1080/07315724.1990.10720349. PMID2407766.
- ^Charlier, R; Deltour, G; Baudine, A; Chaillet, F (November 1968). 'Pharmacology of amiodarone, and anti-anginal drug with a new biological profile'. Arzneimittel-Forschung. 18 (11): 1408–17. PMID5755904.
- ^Singh, BN; Vaughan Williams, EM (August 1970). 'The effect of amiodarone, a new anti-anginal drug, on cardiac muscle'. British Journal of Pharmacology. 39 (4): 657–67. doi:10.1111/j.1476-5381.1970.tb09891.x. PMC1702721. PMID5485142.
- ^Damato, Anthony N. (1 July 1969). 'Diphenylhydantoin: Pharmacological and clinical use'. Progress in Cardiovascular Diseases. 12 (1): 1–15. doi:10.1016/0033-0620(69)90032-2. PMID5807584.
- ^'The 'Sicilian Gambit'. A new approach to the classification of antiarrhythmic drugs based on their actions on arrhythmogenic mechanisms. The Task Force of the Working Group on Arrhythmias of the European Society of Cardiology'. Eur. Heart J. 12 (10): 1112–31. October 1991. PMID1723682.
- ^Vaughan Williams EM (November 1992). 'Classifying antiarrhythmic actions: by facts or speculation'. J Clin Pharmacol. 32 (11): 964–77. doi:10.1002/j.1552-4604.1992.tb03797.x. PMID1474169.
- ^'Milestones in the Evolution of the Study of Arrhythmias'. Retrieved 2008-07-31.[dead link]
- ^Fogoros, Richard N. (1997). Antiarrhythmic drugs: a practical guide. Oxford: Blackwell Science. p. 49. ISBN978-0-86542-532-3.
- ^Lei, Ming; Wu, Lin; Terrar, Derek A.; Huang, Christopher L.-H. (23 October 2018). 'Modernized Classification of Cardiac Antiarrhythmic Drugs'. Circulation. 138 (17): 1879–1896. doi:10.1161/CIRCULATIONAHA.118.035455. PMID30354657.
Retrieved from 'https://en.wikipedia.org/w/index.php?title=Antiarrhythmic_agent&oldid=891008707'
Prescriptions Being Filled at an All-Time High
Almost 4 billion prescriptions for medications were written in the United States in 2010, an all-time high. Major studies that analyzed the financial impacts of increased therapeutic drug use on treatment outcomes and spending have come to different conclusions. However, it is known that many diseases can be prevented, treated effectively or cured through prescription medications.
'In some cases, the use of prescription medicines keeps people from needing other expensive health care such as being hospitalized or having surgery,' notes the Kaiser Family Foundation.
Nine-out-of-10 senior citizens in the United States and more than half (58 percent) of all non-seniors regularly rely on a prescribed drug, according to the Agency for Healthcare Research and Quality.
All classes of drugs have seen an increase in prescriptions filled over the last 5 years except diuretics, penicillins, and hormonal contraceptives, according to the IMS Institute for Healthcare Informatics. IMS's analysis included all prescription medications dispensed through retail pharmacies, food store pharmacies, mail orders and long-term care facilities.
Generics Surpass Branded Drug Scripts
Generic drugs represented 75 percent of all filled prescriptions in 2010, up from 57 percent in 2004, according to IMS. While the number of generic prescriptions dispensed increased 5.9 percent; branded prescriptions declined by 7.6 percent.
The Most Prescribed Medications by Class
Lipid Regulators
Lipid regulators, mainly statin drugs, are used to prevent dyslipidemia (high blood cholesterol) and other cardiovascular problems and have been prescribed for the prevention and treatment of many other illnesses including osteoporosis and post-menopause complications. More than 255.4 million prescriptions for statins and other lipid-lowering drugs were filled in 2010.
Pfizer's Lipitor (atorvastatin calcium) was the highest selling branded statin, followed by Crestor (rosuvastatin calcium) by AstraZeneca; Other branded statins included Mevacor (lovastatin), Pravachol (pravastatin sodium), Zocor (simvastatin), Lescol (fluvastatin sodium), Vytorin (Ezetimibe/Simvastatin), and Pitavastatin.
Awareness campaigns directed at physicians and directly to consumers have contributed to the growth in this class of drugs.
Antidepressants
Antidepressants are one of the fastest growing classes of prescribed drugs. In 2010, more than 253.6 million prescriptions were filled for antidepressants, according to the IMS report.
One of the main factors driving the increase in scripts for antidepressants is that a growing number of primary care providers and others practicing outside the field of psychiatry are writing the prescriptions for patients who have not received a clinical psychiatric diagnosis, according to a study published in Health Affairs journal in August 2011.
'Our analysis found that between 1996 and 2007, the proportion of visits at which antidepressants were prescribed but no psychiatric diagnoses were noted increased from 59.5 percent to 72.7 percent,' wrote co-authors Ramin Mojtabai, Johns Hopkins Bloomberg School of Public Health, and Mark Olfson, with the College of Physicians and Surgeons of Columbia University in New York, and a research psychiatrist at New York State Psychiatric Institute.
Narcotic Analgesics
Narcotic analgesics are prescribed for the relief of severe pain. In 2010, more than 244,300 prescriptions were filled for these types of painkillers.
Some leading narcotic analgesics include Oxycodone (oxycodone), Vicodin (hydrocodone and acetaminophen), codeine, morphine, Percocet (acetaminophen and oxycodone), and Ultram (tramadol).
Beta-Blockers
Beta-adrenergic blocking agents or beta-blockers (plain and in combination with other drugs, are prescribed for the treatment of heart disease, particularly high blood pressure, as well as glaucoma, hyperthyroidism, and migraines. More than 191.5 million prescriptions for beta-blockers were filled in 2010.
Commonly prescribed beta-blockers include Brevibloc (esmolol), Coreg (carvedilol), Inderal (propranolol), Lopressor, Toprol-XL (metoprolol), Normodyne, Trandate (labetalol), Sectral (acebutolol), Tenormin (atenolol) and Zebeta (bisoprolol).
ACE Inhibitors
Angiotensin-converting enzyme (ACE) inhibitors are used in the treatment of high blood pressure, scleroderma, migraines and other conditions. In 2010, pharmacies dispensed more than 168.7 million prescriptions for ACE inhibitors.
ACE inhibitors include Lotensin (benazepril), Capoten (captopril), Vasotec (enalapril), Fosinopril, Prinivil, Zestril (Lisinopril), Univasc (Moexipril), Aceon (perindopril), Accupril (quinapril), Altace (ramipril) and Mavik (trandolapril).
Other top-ranking classes of drugs by millions of prescriptions filled are:
- 6. Antidiabetes; 165
- 7. Respiratory Agents; 153.3
- 8. Anti-Ulcerants; 147.1
- 9. Diuretics; 131
- 10. Anti-Epileptics; 121.7
- 11. Tranquilizers; 108.6
- 12. Thyroid Preps; 107.2
- 13. Calcium Antagonists (Plain & Combo); 97.9
- 14. Antirheumatics; 95
- 15. Hormonal Contraceptives; 92.3
- 16. Angiotensin II; 83.7
- 17. Penicillins; 76.1
- 18. Macrolides & Similar Type; 73.9
- 19. Vitamins & Minerals; 71.9
- 20. Hypnotics & Sedatives; 66
Source:IMS Health, National Prescription Audit, Dec 2010
Attention deficit hyperactivity disorder (ADHD) is a mental disorder. It causes a range of symptoms. These include:
- forgetfulness
- an inability to finish tasks
Medications can help decrease ADHD symptoms in children and adults. Treatment approaches can vary between children and adults, and not every person with ADHD takes the same drugs.
In fact, many drugs are available to treat ADHD. The following list of drugs for ADHD can help you talk to your doctor about what option may be right for you.
Stimulants are the most commonly prescribed medications for ADHD. They’re often the first course of drugs used for ADHD treatment. You might hear this class of drugs called central nervous system (CNS) stimulant medications. They work by increasing the amounts of the hormones called dopamine and norepinephrine in the brain. This effect improves concentration and decreases the fatigue that’s common with ADHD.
Many brand-name stimulants are now only available as generic versions, which cost less and may be preferred by some insurance companies. However, other drugs are only available as brand-name products.
Amphetamines
Youtube twilight movie part 1. Amphetamines are stimulants used for ADHD. They include amphetamine, dextroamphetamine, or lisdexamfetamine. They come in immediate-release (a drug that’s released into your body right away) and extended-release (a drug that’s released into your body slowly) oral forms. Brand names of these drugs include:
- Adderall XR (generic available)
- Dexedrine (generic available)
- Dyanavel XR
- Evekeo
- ProCentra (generic available)
- Vyvanse
Methamphetamine (Desoxyn)
Methamphetamine is related to ephedrine and amphetamine. It also works by stimulating the CNS. It’s not known exactly how this drug works to help ADHD symptoms. It can reduce your appetite and increase your blood pressure. This drug comes as an oral tablet taken once or twice per day.
Methylphenidate
Methylphenidate works by helping the reuptake of norepinephrine and dopamine in your brain. It’s also a mild stimulant. It comes as immediate-release, extended-release, and controlled-release oral forms. It also comes as a transdermal patch under the brand name Daytrana. Brand names include:
- Aptensio XR
- Metadate ER
- Concerta (generic available)
- Daytrana
- Ritalin (generic available)
- Ritalin LA (generic available)
- Methylin (generic available)
- QuilliChew
- Quillivant
- Focalin (generic available)
Non-stimulants affect the brain differently than stimulants do. These drugs also affect neurotransmitters, but they don’t increase dopamine levels. In general, it takes longer to see results from these drugs than from stimulants.
These drugs come in several classes. A doctor might prescribe them when stimulants aren’t safe or are ineffective. They may also prescribe them if a person wants to avoid the side effects of stimulants.
Atomoxetine (Strattera)
Atomoxetine (Strattera) lets norepinephrine work longer in the brain. The drug is long-acting, so you only need to take it once per day. This drug is also available as a generic.
Atomoxetine has caused liver damage in a small number of people. If you have signs of liver problems while taking this drug, your doctor will check your liver function. Signs of liver problems include a tender or swollen abdomen, yellowing of your skin or the whites of your eyes, or fatigue.
Clonidine (Kapvay)
Clonidine (Kapvay) is used to reduce hyperactivity, impulsiveness, and distractibility in people with ADHD. App store for laptop free. This drug is also used to treat high blood pressure. Because it also lowers blood pressure, people taking it for ADHD may feel lightheaded.
This drug is available as a generic.
Guanfacine (Intuniv)
Guanfacine (Intuniv) is normally prescribed for high blood pressure in adults. This drug is available as a generic, but only the time release version and its generics are approved for use in children with ADHD.
This drug may help with memory and behavioral problems. It may also help improve aggression and hyperactivity.
Your doctor may suggest other ADHD treatments along with medications.
For instance, an article in the journal Pediatrics says that changing your diet may alleviate your ADHD symptoms. A study in Clinical Psychology Review found that taking omega-3 supplements may also modestly improve symptoms in children with ADHD. Talk to your doctor about your drug options as well as the alternatives, such as these six natural remedies. It’s important to discuss all ADHD treatment options with your doctor to gain the best results.
Q:
Are the same drugs that are used to treat ADHD in children used to treat adult ADHD?
A:
Yes. However, the dosages of many of these drugs are different for kids than they are for adults. Also, the side effects of these drugs are different in adults than they are in children. Your medical history can limit your treatment options. It’s important to talk to your doctor about your medical history to get an idea of which of these drugs is likely to work best for you.
Healthline Medical TeamAnswers represent the opinions of our medical experts. All content is strictly informational and should not be considered medical advice.
